NYTimes is now Pro-Obesity & Mt Sinai Med School Says Weight Loss is Racist: Medicine is Drowning in Deranged Ideas.
We need to stand up for common sense in medicine
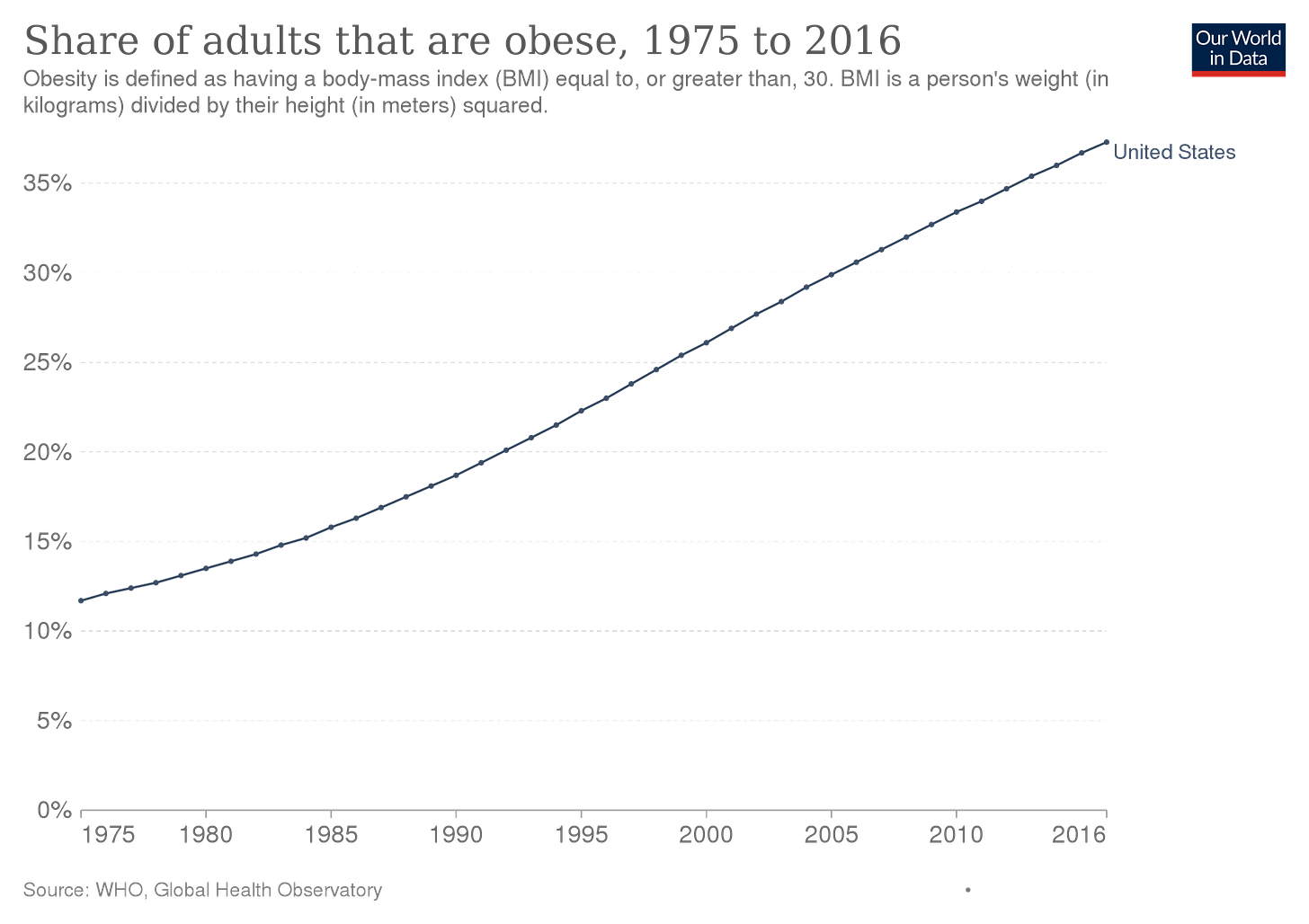
This week, I read two things that are emblematic of just how common sense is in a decline in American medicine. They are both on the topic of obesity. First, let’s remind ourselves that obesity is a problem that is rapidly getting worse in America. We are fatter than ever before.
Now, if I were in charge of federal budgets, I would commission dozens of large, 10k-100k randomized trials of different dietary and exercise strategies, different health advice, different incentives for grocery stores (cluster design), parks (cluster), bike lanes (cluster), and many other interventions.
My trials would be powered for hard endpoints (CV events, death, etc), with supplementary studies powered for HRQoL and softer endpoints among the young. If medications are tested, particularly in younger people, I would expand the sample size to 100k+, and extend duration of follow to look for rare and relevant safety signals that might be missed.
You know what I wouldn’t do: Deny that it is a problem.
Exhibit A: Mt Sinai school of medicine has emailed the entire school, arguing that diet culture is racist. I attach the full email at the bottom of this essay, so you can see for yourself just how ridiculous it is.
The argument made is that the idea ‘it is good to be thin’ is itself racist, and the general argument advanced is that Black and Brown communities often live in food deserts, and there are fewer dietitians who are familiar with preferred foods of these groups to give relevant advice.
But the authors are making a flawed argument. Yes, we should work on making healthy foods equally available to all Americans, irrespective of race and wealth. And yes, we should work on having a variety of dietary advice that pleases all palettes. And yes, we should study the optimal weight and BMI for different people by race or ethnicity, body type and other factors, but the idea that ‘being thin is healthy’ is not racist. The path to get there may be harder for some people, but the goal is sound for all races.
Finally, why are they emailing this to the entire school of medicine? Why is there no rebuttal? What are they teaching medical students? (is it teaching if you don’t entertain debate on demonstrably false claims?)
Exhibit B: The New York Times has an essay critical of the New Pediatric Obesity guidelines. My first thought— was good! I was also critical about putting a 12 year old boy on a GLP1 agonist weight loss drug in perpetuity. Does he take it for 50 years? What AEs happen with 50 years of treatment? But I was wrong!
The article was critical of the very fact that obesity is bad.
The author argues that Obesity is not a problem in kids. And that we could embrace different weights. She even gives the most bizarre advice I have ever seen for an Obese person: eat more calories!
Have we lost our minds?
Of course, no one should be teased or mocked or treated poorly because of their weight. And children are sensitive, and issues of weight should be discussed compassionately and carefully, but if you want to claim that it is good that kids’ weight is rising, and obesity is the highest it has ever been— you are out of your mind.
It is neither racist nor bad medicine to try to compassionately get someone who is overweight or obese to lower their weight. Their blood pressure may fall; They may have more energy; COVID is less likely to kill them; and they may live longer.
Just how to best counsel them is an open question— requiring RCTs (and huge ones)— but the idea that this is a task worth taking is settled. Obesity is unhealthy; The rise in obesity is bad for health and humanity; and we have to tackle it.
Minorities and poor people need extra support, but they do not need to be told the very premise of losing weight is racist or unnecessary. Kids need much better evidence— and, yes, the AAP is a terrible organization that just makes things up— but the idea obesity is harmful to kids is true.
Medicine is suffering from a brain parasite: the ideas expressed in both these essays. Trying to lower weight among those with unhealthy weight is a racist goal, and we should be happy with surge in obesity among children—- These are clearly ridiculous ideas that are being presented as if they are fact with little push back.
Common sense in medicine is dying.
Full Exhibit A:






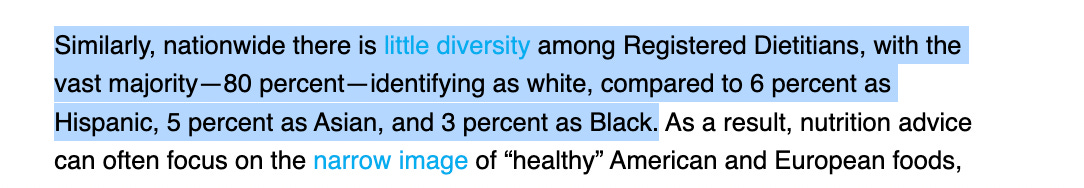





Either you didn't read the NYT piece, or you're being purposely obtuse. The author states, correctly, that our current measures for weight loss (for everyone, including kids) don't work. She also states, again correctly, that the BMI is not a reliable measurement when used in kids. And yet, the new AAP guidelines focus on BMI for *two year olds*.
Is obesity in kids a problem? Maybe. Should we treat it as aggressively as the AAP suggests? Heck no. As Emily Oster writes in her piece (https://www.parentdata.org/p/new-aap-guidelines-on-childhood-obesity) on the new guidelines, "There is a link between childhood obesity and adult obesity, but the predictive power is not 100%. About half of children with obesity go on to have obesity in adolescence, and about 70% of adolescents with obesity go on to have obesity at age 30."
Yet we have the AAP recommending weight loss medications and bariatric surgery - permanently altering the bodies of children as young as 13. Whose ideas are deranged again?
Rats. I really think diving into the data on obesity would be your jam Vinay. That being fat is bad for us is just the kind of thing that’s so obvious to us that we don’t need data to believe it. The kind of thing I know you are keen to investigate further. When I’ve gone back and looked at the highest quality data we have I’ve been left with the impression that the downsides of obesity are far overstated, especially for the BMI 30-35 group (the vast majority of “obese” people). I’ve come to wonder if fat bias isn’t more detrimental than fatness itself. It’s certainly true that telling folks to lose weight, which we’ve been doing for decades, hasn’t done anything to move the needle (or perhaps it has, and it’s backfiring!). I worry you’re not taking your usual approach to this issue. Yes, we need RCTs, but the question should be “do people live better and/or longer if they lose weight with X intervention?” And we must be open to the possibility that our interventions may lead to weight loss without improvement in morbidity or mortality, because perhaps being fat per se isn’t bad at all.